
- Home
- News
- Analysis
- States
- Perspective
- Videos
- Education
- Entertainment
- Elections
- Sports
- Features
- Health
- Budget 2024-25
- Business
- Series
- Bishnoi's Men
- NEET TANGLE
- Economy Series
- Earth Day
- Kashmir’s Frozen Turbulence
- India@75
- The legend of Ramjanmabhoomi
- Liberalisation@30
- How to tame a dragon
- Celebrating biodiversity
- Farm Matters
- 50 days of solitude
- Bringing Migrants Home
- Budget 2020
- Jharkhand Votes
- The Federal Investigates
- The Federal Impact
- Vanishing Sand
- Gandhi @ 150
- Andhra Today
- Field report
- Operation Gulmarg
- Pandemic @1 Mn in India
- The Federal Year-End
- The Zero Year
- Premium
- Science
- Brand studio
- Newsletter
- Home
- NewsNews
- Analysis
- StatesStates
- PerspectivePerspective
- VideosVideos
- Entertainment
- ElectionsElections
- Sports
- Features
- BusinessBusiness
- Premium
- Loading...
Premium - India-Canada ties
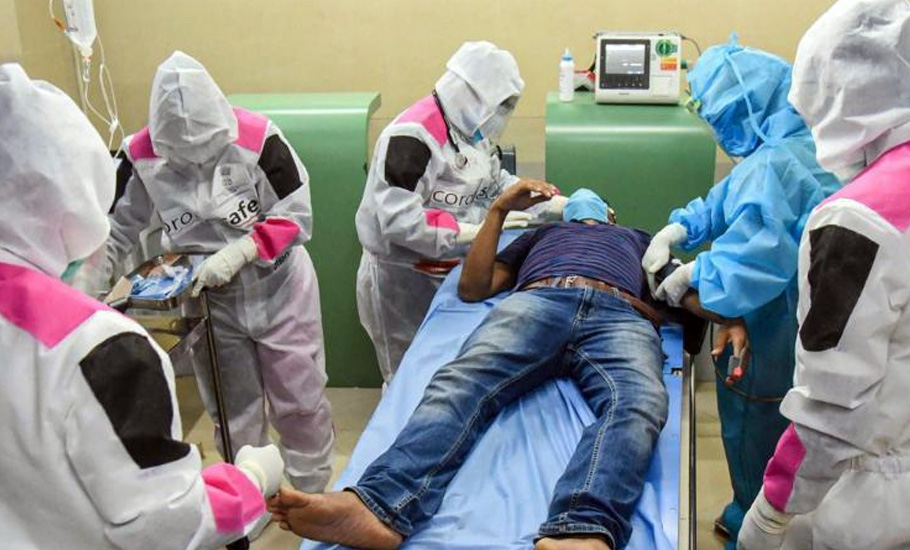
Life after COVID: The fatigue, the isolation and the haunting anxiety
Undergoing treatment at Kerala's COVID first line treatment centre (CFLTC) can be an exhausting experience, that leaves patients isolated and distressed.

It’s been more than 10 days since 78-year-old Suhasini returned from the COVID First-Line Treatment Centre (CFLTC) at Muttambalam Block Panchayat in Kerala’s Kottayam district. Her movements are slow lest the fatigue should come back; her appetite is normal but her sense of taste is yet to return; and she never had the fever anyway. But Suhasini doesn’t feel lucky. She doesn’t even...
It’s been more than 10 days since 78-year-old Suhasini returned from the COVID First-Line Treatment Centre (CFLTC) at Muttambalam Block Panchayat in Kerala’s Kottayam district.
Her movements are slow lest the fatigue should come back; her appetite is normal but her sense of taste is yet to return; and she never had the fever anyway. But Suhasini doesn’t feel lucky. She doesn’t even smile, because her maid of 16 years refuses to enter the house.
“We thought that we would have a horrible time being sick under the state government’s care,” she says. “But that was a breezy stint when compared to what we are going through now.”
She is not exaggerating. The Kerala government is one of the very few governments in the world that has complete monopoly over its post-pandemic public health system.
“People ask why this government is so invested into its own public health when the effect of the pandemic is the same everywhere,” says Dr Mohammed Asheel, executive director of Kerala Social Security Mission. “I tell them that it is because there’s only one question that is asked at the end of every epidemic in history – ‘How many lives could you have saved and at what cost’?”
The state has a three-pronged strategy for COVID-19 patient management. The first option comprises the CFLTCs, the tertiary care centres and medical colleges. Category A patients with mild symptoms like low-grade fever and general fatigue go to the CFLTCs at the block levels, which are usually multi-storey government accommodations. Category B patients with co-morbidities like diabetes/ cardiac issues/ malignancy go to Tertiary Care Centres, which are district and taluk hospitals. Category C is solely for those who need critical care — the ICU wards in medical colleges and general hospitals.
The second option is special private hospitals for all three categories, at one’s own expense, and the third is home quarantine, meant only for the asymptomatic.
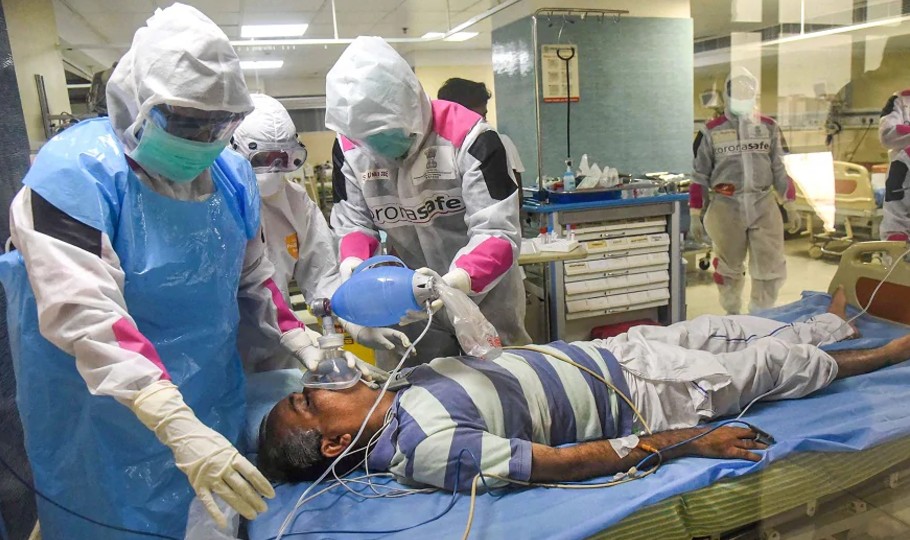
Inside the facility
When Suhasini and her family of five tested positive and opted for the free government care, the district health department officer told them they had two choices — one was a CFLTC that had 20-bed dormitories on each floor and the other was a roomed facility, both without attached bathrooms or dining halls.
They chose the latter and fortunately, two rooms were vacant on a triple-sharing basis. “We were told to pack as if we were going on a trip; the only add-ons were an induction cooker, kitchen utensils and buckets.”
Food is served four times a day. Breakfasts include dosa, idli, puttu; lunch is always rice and curry with fish daily: tea with a snack; and dinner is rice gruel or chapati with curry.
The resident doctor makes his rounds twice a day; vitals are checked and vitamin supplements are administered. Every inmate does steam inhalation and saline gargle multiple times a day, mostly with their own water-heating devices.
Suhasini had fever for one day. After that, she was totally asymptomatic. Her son, however, was diabetic and so had mild body pain for the first few days. Both her grandchildren, aged 24 and 20, had no symptoms.
On the 11th day, they were discharged after their second antigen test.
“The men-folk stay up late at night playing cards. The women are always almost on the phone,” says Meena, Suhasini’s daughter-in-law. “Masks and social distancing are a must at all times.”
Bathrooms are assorted according to the room numbers. “Everywhere you looked, written instructions were pasted on the walls.”
As of now, around 240 CFLTCs in the state run with 60% occupancy.
Things were not the same for others. Jisha Cherian, another COVID patient in the region, took one long look at the CFLTC the ambulance took her to and had a meltdown. She was overweight and already had respiratory issues. “I was the only positive member in my family then.”
The bathrooms assorted to her dormitory were on a different floor. “No dining hall meant that I would have to sit on the bed and balance the plate on my lap.”

She called her councillor and asked to be taken to another CFLTC that had rooms. But there was no vacancy. So she called her councillor again.
“This time, I opted for a private hospital.” At the end of 10 days, she and her husband (who got admitted in the adjacent deluxe room three days later) shelled out ₹1,20,000. She has no regrets. In fact, she highly recommends it for those with the ‘purchasing power’.
Dr Anup Warrier, the COVID-19 in-charge at a super-specialty private hospital in Cochin, says, “Our First Line Treatment Centre facility for category A costs approximately ₹7000 a day. We have 24 rooms on double occupancy, with air conditioning and a round-the-clock menu.”
Six nurses on three separate shifts along with a general physician who does two rounds daily attend to the patients. Every floor segregated for COVID treatment has physical barriers for entry/exit and an independent air handling unit.
The 60-bed facility for category B patients cost anywhere between ₹10,000–12,000 per day. Category C is an exclusive 20-bed ICU unit that can set one back by ₹30,000–40,000 a day. “We have only 60% occupancy for the CFLT but both our high-end units were running full by mid-September and have long waiting lists,” Dr Warrier says.
Home isolation
On the other hand, home isolation is also fast becoming a popular option as asymptomatic persons are relatively healthy.
The concerned medical officer in the area needs to ensure that the infected are physically and psychologically fit and that their homes can function as isolated spaces. Follow-up is done mainly through the telephone or by visits. The well-to-do even buy gadgets like pulse oximeters to record their readings daily.
“The problem here is that many families are choosing to do this quietly and independently”, says Dr Gopakumar, lab surveillance officer with the district COVID control cell. “But an unmanned spike in breathlessness can catapult them straight to category B or C.”
Here again, the state is making heavy intervention. “For the marginalised who go hungry or do not have a proper home, we will soon be introducing Domiciliary Centres,” says Dr Asheel. “Hostel-like accommodations with food and medicines would be provided free by the respective panchayats, but without any medical supervision.”

Through anxiety and distress
But comfort and luxury can only mean so much. “The overall feeling of patients at COVID centres is one of anxiety”, says Dr Tony, junior consultant in psychiatry, general hospital.
Dr Tony tested positive while on duty and chose to be in isolation at the medical college in his district. “As a physician on COVID duty, I knew this disease was not a medical threat. I’ve fallen ill to dengue and H1N1. Those were extremely painful and serious health risks. But Covid-19 is not invasive; one can live along with it. The isolation and the stigma, however, can take a very heavy toll.”
Dr Tony’s anxiety stemmed from the fact that his wife and children had no secondary family to take care of them while he was in hospital.
For Jisha, the anxiety took a toll on her sleep. She hardly slept during the seven days that she stayed in her single deluxe room.
“I would wake up 3-4 times at night. I had no sense of taste, so I wasted most of my food. The rest of my family was positive but under home isolation. The guilt that they got it from me added to my misery.”
For 58-year-old Anil, all he could think of during his isolation period was how he could have even gotten this virus. “I was so careful. Even the pen that I used at work was washed in Dettol everyday!”
“Normal stress is helpful. It allows you to overcome your trauma. But when stress becomes distress, it needs to be spotted,” says Dr Merin Poulose, in-charge of the Psychiatric Social Support team in Wayanad. “Patients have been reported to have anxiety-induced deliriums and withdrawal symptoms.”
This is why the state government has now allowed one member of the family to be a by-stander inside category C facilities. In fact, every CFLT centre has an in-house mental health professional on call when a patient starts acting up.
The biggest trauma, however, is when they return to their homes completely cured.
Suhasini is still smarting from the responses of her maid, her neighbours and even the milkman. “He told us to use our own bottles. His containers won’t be available from now on.”
Jisha has returned home but her doctor told her to take it easy for at least three months. “My health will come back. But I’m not that sure about people’s feelings.”
Most returnees from the CFLTCs and hospitals have chosen to stay in quarantine longer than they were expected to. “Only to reassure our neighbours and community that we are not a health risk at all,” says Das, 62. Almost all have rejoined work too.
Apparently, Suhasini was right. Getting rid of a disease without having to spend a penny was not the challenge. Getting one’s life back, that is the uphill task.

