Hydrogen Sulphide gas may help tackle HIV: Study

A more comprehensive treatment for Human Immunodeficiency Virus (HIV) infection could be in the offing. A study has found that the pungent hydrogen sulphide (H2S) gas could help reduce the rate at which the virus multiplies in infected human immune cells.
The current state-of-the-art treatment for HIV is a combined antiretroviral therapy (cART). It is, however, not a cure. It only suppresses the virus, making it become latent. Certain negative effects are also associated with cART, such as the build-up of toxic molecules leading to oxidative stress and loss of function in the mitochondria, the cell’s powerhouse. These effects can contribute to inflammation and organ damage.
The new study, which was conducted by researchers from the Department of Microbiology and Cell Biology (MCB) and the Centre for Infectious Disease Research (CIDR) at the Bengaluru-based Indian Institute of Science (IISc), and their colleagues from the Bangalore Medical College and Research Institute, could help tackle this issue.
In a previous study, the laboratory of Amit Singh, Associate Professor in MCB/CIDR and corresponding author of the new study, developed a tool to measure oxidative stress in cells infected with HIV. In that work, the scientists showed that a chemical agent called N-acetylcysteine was able to suppress HIV reactivation from latently infected cells.
Also read: Study by Pune-based DBT-NCCS finds new therapeutic target for cancer
A German study later showed that N-acetylcysteine partly acts by releasing H2S molecules. “Since H2S also functions as an antioxidant molecule, we wished to see whether our prior insights on oxidative stress and HIV could be translated to show the contribution of H2S on HIV infection,” the study said.
As the study on the role of H2S in HIV has begun only recently, the authors had to set experiments up from scratch. “Studying the effects of a gaseous molecule on HIV required us to build and validate new model systems,” says Virender Kumar Pal, a PhD student in MCB and the first author of this study.
The researchers studied the effects of the natural generation of H2S in HIV-infected cells as well as supplementing this with a chemical donor.
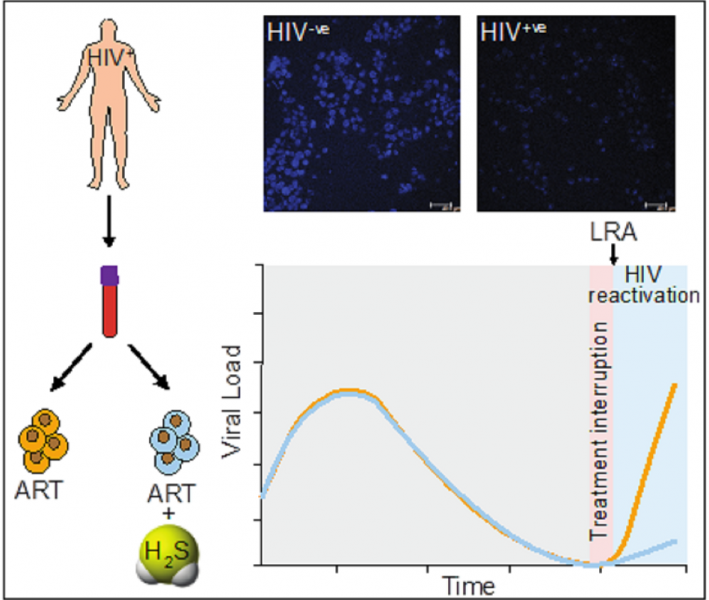
“We observed a direct effect of H2S on suppressing HIV reactivation and replication along with all its other beneficial effects, such as maintenance of mitochondrial health and dissipation of oxidative stress in our [cellular] models,” said Singh. “Our results suggest that maintenance of HIV latency and reactivation are closely linked to the H2S levels in infected cells.”
Also read: Study led by IIT Mandi professor gains new insights into Alzheimer’s
The study, he said, could open the door to supplementing cART with chemical donors of H2S to lock HIV in a state of deep latency, potentially improving the lives of millions infected with the virus. Since H2S donors are already undergoing clinical trials for other diseases, they can quickly be repurposed for HIV treatment. The researchers have published their findings in the journal eLife. The team included R. Agrawal R, S.Rakshit, P.Shekar, D.T.N.Murthy and A. Vyakarnam.


