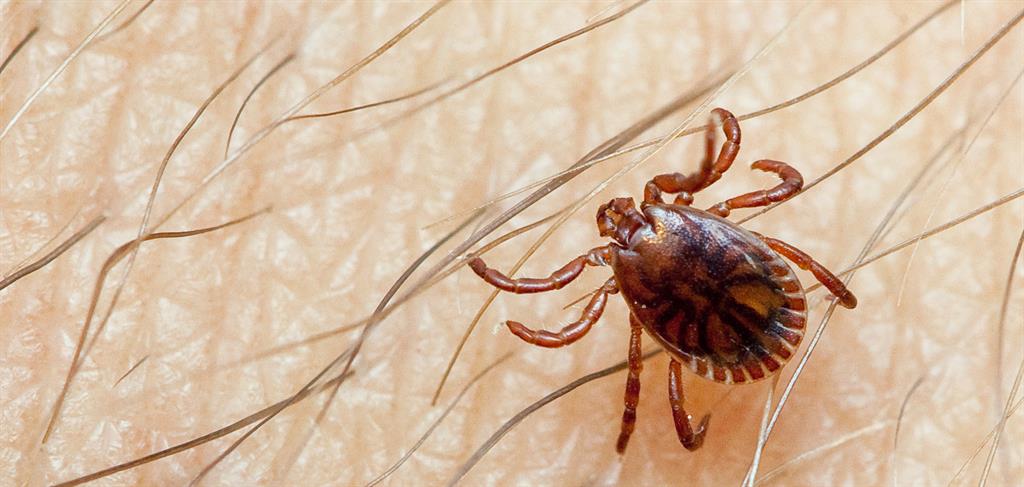
Nose-bleed fever hits India. Find out its symptoms, precautions

Iraq has witnessed an outbreak of nose-bleed fever or Crimean-Congo haemorrhagic fever (CCHF) and so far this year 212 cases were detected and 27 people have died. India has now reported two cases from Gujarat and one death.
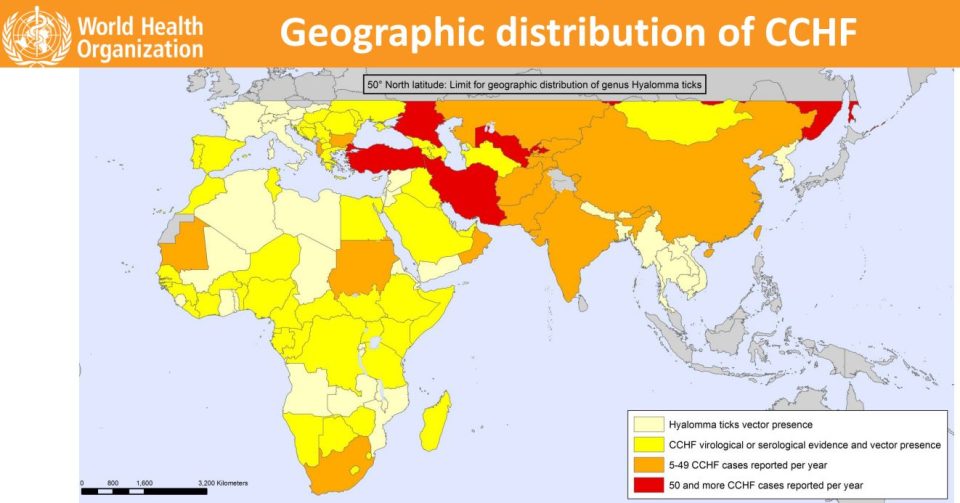
According to the World Health Organization (WHO), nose-bleed fever is endemic in Africa, the Balkans, the Middle East and Asia.
Also read: What is toe jam? From harmless gunk to a feast for bugs
As per its estimates, 3 billion people are at risk with 10,000 to 15,000 infections every year and an estimated 500 deaths each year.
The first CCHF case in India was reported in 2011 from Gujarat. According to the WHO’s geographic distribution of nose-bleed fever cases, India reports 5 to 49 infections each year.
What is CCHF?
Crimean-Congo haemorrhagic fever is a viral haemorrhagic fever usually transmitted by ticks. It can also be contracted through contact with viraemic animal tissues (animal tissue where the virus has entered the bloodstream) during and immediately post-slaughter of animals, according to the WHO.
CCHF outbreaks constitute a threat to public health services as the virus can lead to epidemics, has a high case fatality ratio (10-40%), potentially results in hospital and health facility outbreaks, and is difficult to prevent and treat, it added.
Also read: Pregnancy, childbirth & COVID: Find answers to commonly asked questions
“The hosts of the CCHF virus include a wide range of wild and domestic animals such as cattle, sheep and goats. Many birds are resistant to infection, but ostriches are susceptible and may show a high prevalence of infection in endemic areas, where they have been at the origin of human cases. For example, a former outbreak occurred at an ostrich abattoir in South Africa. There is no apparent disease in these animals.
“Animals become infected by the bite of infected ticks and the virus remains in their bloodstream for about one week after infection, allowing the tick-animal-tick cycle to continue when another tick bites. Although a number of tick genera are capable of becoming infected with the CCHF virus, ticks of the genus Hyalomma are the principal vector,” the WHO explained.
The disease was first described in Crimea in 1944 and given the name Crimean haemorrhagic fever. In 1969 it was recognised that the pathogen causing Crimean haemorrhagic fever was the same as that responsible for an illness identified in 1956 in the Congo. The linkage of the two-place names resulted in the current name for the disease and the virus.
Video: Centre, states on high alert for monkeypox
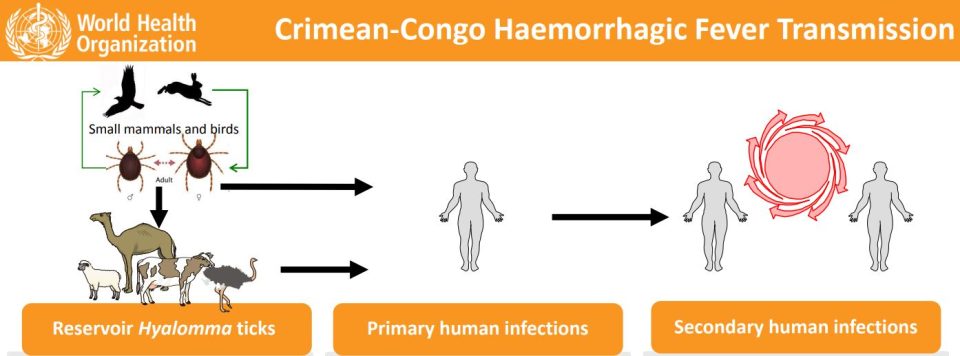
Primary human infections
The WHO said that CCHF is a viral tick-borne disease that is transmitted to humans by bites of infected ticks, and by direct contact with blood or tissues from infected humans and livestock. About 80 to 90 % of humans are infected through tick bite or direct contact with blood of infected ticks; direct contact with blood/tissues of infected wild animals and livestock. Secondary human-to-human transmission occurs through direct contact with the blood, secretions, organs or other body fluids of infected persons. High transmission risk when providing direct patient care or handling dead bodies (funerals).
Also read: Study shows high possibility of blood clotting up to 6 months post-COVID
The WHO said that studies have shown sheep and cattle husbandry are regularly infested with tick species, mainly Hyalomma species, the principal vector of CCHF.
Ticks’ sizes
Ticks live in the ground vegetation and move mainly by climbing up plants and walking on the ground. They latch on to a passing animal or human host by using hooks on their legs. The sizes of ticks can vary from 0.5 to 15 mm, depending on tick species.
Symptoms
Also read: WHO: Nearly 200 cases of monkeypox in more than 20 countries
Most common symptoms include abrupt onset fever, chills, shudders, myalgia, headaches, sicknesses and vomits, abdominal pain, arthralgia. After a few days – bleeding from mucous membranes, hematomas, ecchymosis, melena, hematuria, nose bleeding, vaginal bleeding, bradycardia, thrombocytopenia, leukopenia, according to the WHO.
The length of the incubation period depends on the mode of acquisition of the virus. Following infection by a tick bite, the incubation period is usually one to three days, with a maximum of nine days. The incubation period following contact with infected blood or tissues is usually five to six days, with a documented maximum of 13 days, said the WHO.
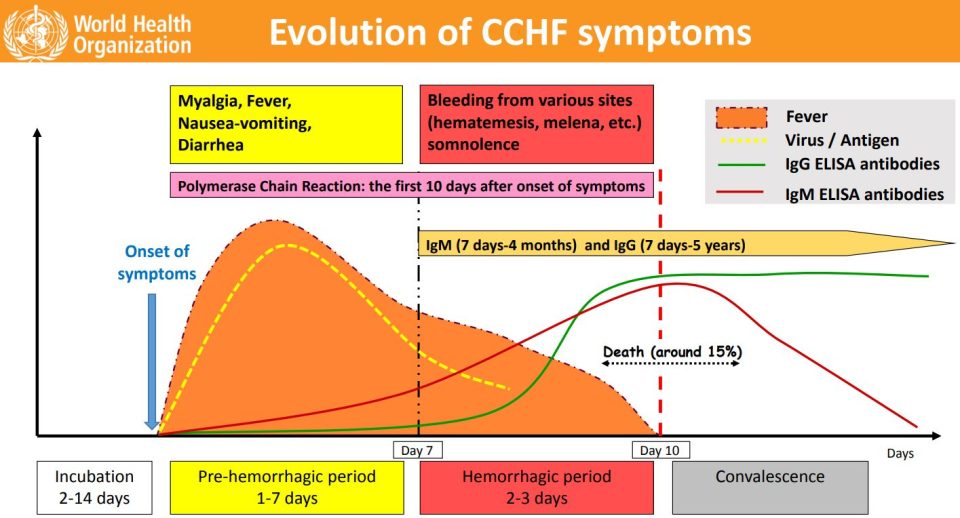
Other clinical signs include tachycardia (fast heart rate), lymphadenopathy (enlarged lymph nodes), and a petechial rash (a rash caused by bleeding into the skin) on internal mucosal surfaces, such as in the mouth and throat, and on the skin. The petechiae may give way to larger rashes called ecchymoses, and other haemorrhagic phenomena. There is usually evidence of hepatitis, and severely ill patients may experience rapid kidney deterioration, sudden liver failure or pulmonary failure after the fifth day of illness.
Mortality rate
The mortality rate from CCHF, as per the WHO, is approximately 30%, with death occurring in the second week of illness. In patients who recover, improvement generally begins on the ninth or tenth day after the onset of illness.
Treatment
General supportive care with treatment of symptoms is the main approach to managing CCHF in people and the antiviral drug ribavirin has been used to treat CCHF infection with apparent benefit. Both oral and intravenous formulations seem to be effective, as per the WHO.
No vaccines available
The WHO said that there are no vaccines widely available for human or animal use. In the absence of a vaccine, the only way to reduce infection in people is by raising awareness of the risk factors and educating people about the measures they can take to reduce exposure to the virus.
Reducing the risk of infection in people
To reduce the risk of tick-to-human transmission, the WHO recommends the following:
Avoid tick-infested areas; wear protective clothing (long sleeves, long trousers); wear light coloured clothing to allow easy detection of ticks on the clothes; use approved acaricides (chemicals intended to kill ticks) on clothing; use approved repellent on the skin and clothing; regularly examine clothing and skin for ticks; if found, remove them safely; seek to eliminate or control tick infestations on animals or in stables and barns; and avoid areas where ticks are abundant and seasons when they are most active.

To reduce the risk of animal-to-human transmission – wear gloves and other protective clothing while handling animals or their tissues in endemic areas, notably during slaughtering, butchering and culling procedures in slaughterhouses or at home; quarantine animals before they enter slaughterhouses or routinely treat animals with pesticides two weeks prior to slaughter.
Also read: How genetic fingerprints can help doctors diagnose rashes more effectively
To reduce the risk of human-to-human transmission in the community – avoid close physical contact with CCHF-infected people; wear gloves and protective equipment when taking care of ill people; wash hands regularly after caring for or visiting ill people.
India’s preparations
Dr. Samiran Panda, additional Director-General, Indian Council of Medical Research (ICMR), told The Indian Express that the government was fully prepared to deal with any possible outbreak of CCHF. “As far as cases from Iraq are concerned, severe bleeding, both internally and externally, especially from the nose, was observed among two-fifths of the deceased. These are typical symptoms of CCHF cases irrespective of the geographical region,” Dr. Panda said.
“Since 2011, the laboratory screening of CCHF for humans, animals and ticks has been underway. A state-of-the-art containment BSL-4 facility of ICMR at Pune in 2012 made it possible to quickly develop indigenous serological assays for the diagnosis of IgM and IgG for humans and IgG for livestock. These indigenous technologies not only helped in the timely diagnosis of suspected CCHF cases but also in surveillance of CCHF in humans, livestock and ticks in the country,” senior ICMR scientists told the newspaper.


