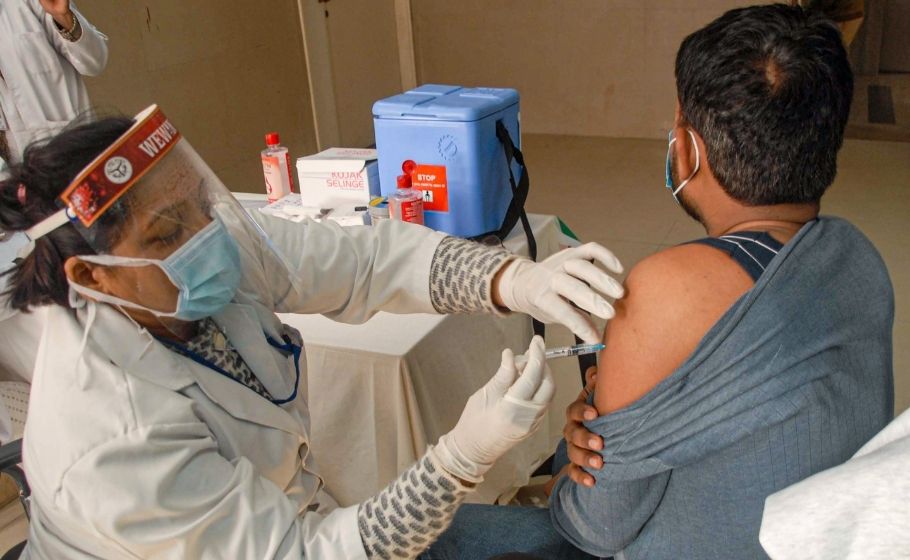
How Kerala has zero vaccine wastage and gets more from its vaccine vials
When there is a crying shortage of vaccines in the country, and as COVID-19 cases continuing to spike, the spotlight is turning on the need to encourage vaccine wastage in states. In April, Tamil Nadu had reported the highest vaccine wastage of 12%, while Kerala had recorded zero wastage.

When there is a crying shortage of vaccines in the country, and as COVID-19 cases continuing to spike, the spotlight is turning on the need to encourage vaccine wastage in states. In April, Tamil Nadu had reported the highest vaccine wastage of 12%, while Kerala had recorded zero wastage.
In fact, Kerala Chief Minister, Pinarayi Vijayan proudly tweeted on May 4 (Tuesday) that though the Centre had supplied 73,38,806 doses of vaccine to the state, they managed to administer 74,26,164 vaccine shots, “even making use of the extra dose available as wastage factor in each vial”. This means they ended up giving an extra 87,358 jabs to people.
Vaccine wastage
So, what is vaccine wastage? According to media reports, sometimes, it is common practice for vials to have extra vaccines, which is known as an overfill. This is to compensate for any spillage or wastage that may occur while the vaccine is being administered. An overfill will mostly be the leftover vaccine in a vial, or it can also be when the vaccine is trapped in a dead space – between the syringe and the needle.
Also read: Only way to control pandemic is by ramping up vaccination drive: Experts
Wastage can also occur when once a vial is punctured, it must be utilised within four to six hours or it has to be discarded. In January, the size of the Covaxin vial was reduced to contain 10 doses instead of 20. The general rule is that a vial is opened only if 7-8 people are available to be vaccinated from it.
In some states like Kerala, the health staff only opens vials when there are enough people to vaccine – there are usually 10 doses in a vial. Sometimes, vaccination centres in the state may send back people if the number is not met, said news reports.
Kerala model of zero wastage
A robust vaccination legacy, strict implementation of protocols for storage, transportation and usage, trained health staff including ASHAs who are frontline social workers and efficient inventory management, has helped Kerala to greatly reduce its wastage. The directive that is given to the field staff is that the vaccine is a scarce product and they need to ensure that everyone receives it.
One of the reasons Kerala is able to reduce vaccine wastage is because the frontline healthcare workers are trained to precisely extract the vaccine from the vial using low dead space syringes. According to a report in News Minute, in Kerala’s stock, each vial can offer 10 doses, but it also contains 0.58 to 0.62 ml (16 to 24%) of overfill, and it is from here they manage to get 11 to 12 doses from a 10-dose vial.
Since residual vaccine from one vial cannot be mixed with vaccine from another vial and administered, Kerala reportedly allots a set number of people for each vial during vaccination drives. Newspaper reports stated that if health centres had only one person left and one vial, they would go out and convince more people to come in and take the vaccine. Kerala had also opened regional vaccine storage centres, so that when the vaccine arrives in the state, they were dispatched to these regional centres to be kept in cold storage.
Also read: States fight back on differential pricing for vaccines, say Centre passing buck
According to the Indian Medical Association involved in vaccination promotion and coordination, vaccine wastage was reported in many states because of their failure to establish regional vaccine centres in each district and evenly distribute the vaccines. Kerala’s success in curbing vaccine wastage has been attributed to the several regional centres that were quickly set up across the state.
The Centre’s COVID-19 vaccine operation guidelines allow for a programmatic wastage of 10 per cent, which is similar to the wastage factor in DPT vaccine, tetanus and PCV. This means that if 100 vials are needed, the stock demand must be of 110 vials assuming there will be a wastage of 10. By factoring in wastage, states like Kerala were able to inoculate more beneficiaries.
To avoid vaccine wastage
Axccording to the health experts, therefore daily vaccination drives must be well mobilised and planned, vials must be opened only after 10 beneficiaries arrive, adequate training must be given to healthcare workers on how to draw doses and to mobilise beneficiaries by instilling confidence in them about vaccines.
It may be interesting to note that Israel, which has vaccinated 56 per cent of its population against COVID-19 last month, had a strategy to avoid wastage when its elderly population was being vaccinated – its youth could walk into immunisation centres towards the end of the day and get vaccinated with the underused vials.


