
- Home
- News
- Analysis
- States
- Perspective
- Videos
- Education
- Entertainment
- Elections
- World Cup 2023
- Features
- Health
- Business
- Series
- Economy Series
- Earth Day
- Kashmir’s Frozen Turbulence
- India@75
- The legend of Ramjanmabhoomi
- Liberalisation@30
- How to tame a dragon
- Celebrating biodiversity
- Farm Matters
- 50 days of solitude
- Bringing Migrants Home
- Budget 2020
- Jharkhand Votes
- The Federal Investigates
- The Federal Impact
- Vanishing Sand
- Gandhi @ 150
- Andhra Today
- Field report
- Operation Gulmarg
- Pandemic @1 Mn in India
- The Federal Year-End
- The Zero Year
- Premium
- Science
- Brand studio
- Home
- NewsNews
- Analysis
- StatesStates
- PerspectivePerspective
- VideosVideos
- Entertainment
- ElectionsElections
- Sports
- Loading...
Sports - Features
- BusinessBusiness
- Premium
- Loading...
Premium
How Covid-19 is keeping patients sleepless and anxious
More and more COVID-19 patients are complaining of sleeplessness, anxiety and depression, among other symptoms, especially among patients admitted to hospitals, and in quarantine.

It has been a month since 35-year-old Bibin was discharged from the Covid-19 isolation ward of a super-specialty hospital in Thiruvalla, Kerala. Medically, he is normal but he still calls the hospital and reports one grievance – he cannot sleep. According to his duty doctor, Bibin was severely agitated and restless from the day he was admitted. Every day, grabbing both of the doctor’s...
It has been a month since 35-year-old Bibin was discharged from the Covid-19 isolation ward of a super-specialty hospital in Thiruvalla, Kerala. Medically, he is normal but he still calls the hospital and reports one grievance – he cannot sleep. According to his duty doctor, Bibin was severely agitated and restless from the day he was admitted. Every day, grabbing both of the doctor’s hands, he would ask – What if I become breathless while sleeping? Shouldn’t I lie awake then?
After discharge, he was required to stay in quarantine at home for another seven days. Those days, he would call the hospital more than twice a day. A month later, his calls are less frequent and his questions have changed. But the fear is still there. Bibin’s family has been advised to get him psychiatric counselling if his anxiety and paranoia persists after three months. Meaning, it will be a very long time till Bibin gets to sleep like a normal person again.
In a clinical profile of psychiatric consultations of in-patients from a Covid Tertiary Centre (June 2020-June 2021), around 118 cases were documented. In a specific analysis of liaison with Category B and Category C patients in Covid wards and ICUs, majority cited anxiety and depressive symptoms “that was overwhelming” and 21 patients with no major disorder were seeking help for illness-related distress.
Withdrawal and isolation
“Unlike other medical treatment units, the Covid-19 facility demands isolation, invasive ventilation, de-personalising behaviour from both staff and the inmates,” says Dr Varghese Punnoose, HOD, Psychiatry, Kottayam Medical College.
Although this treatment protocol is severe but necessary, many non-medical factors go undetected, adding to the increased anxiety and restlessness of the patient.
For instance, withdrawal symptoms among addicts. “Most are concerned only with alcohol addicts. But a Covid patient who is addicted to tea or coffee or cigarettes can also be as easily disturbed. A caffeine addict will keep yawning when he doesn’t get his regular fix, but he is not sleepy. This automated yawning can agitate the patient and mess with his sleeping patterns while in the hospital.”
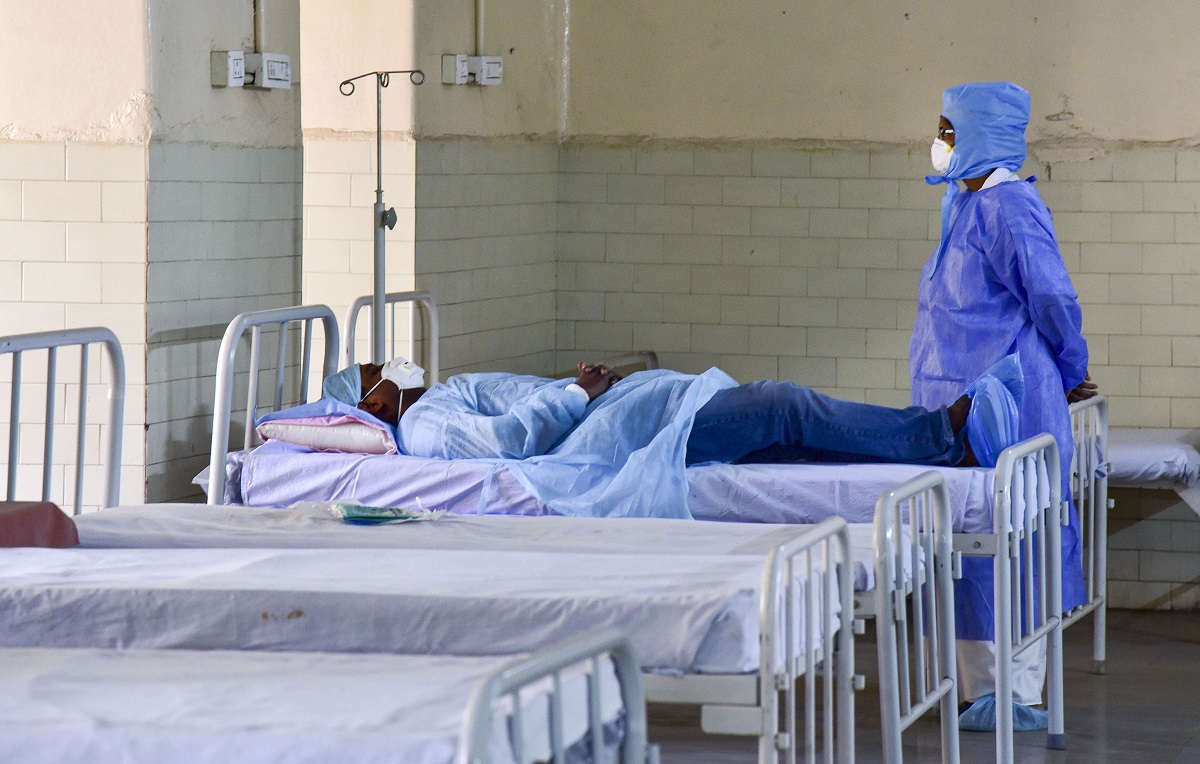
Recalls Seetha M Nair, nursing supervisor at the Believers Church Medical College Hospital, (BCMCH), “Sleeplessness is a huge issue for our patients in both the High Dependency and the Isolation Ward units. We can see them awake at 2 am and 4 am. Those in the HD units do not know the difference between day and night. Complaints of body pain or chest congestion and dry cough are situations we are trained to deal with. But trying to talk them out of their loneliness, fear of dying in their sleep, grief over a recent death in the family takes a toll on us too.”
Seetha says she gets umpteen requests for sedatives from her patients. “Sleepless for more than three consecutive nights is definitely torturous and some of them beg us for sleeping tablets. It is a daily occurrence but we are totally helpless. All we can tell them is to avoid napping during the day as much as possible. Those who are medically fit to sit up or walk to the bathrooms are a little better-off.”
Patients as witnesses
Another unusual occurrence in Covid wards is that patients are also witnesses. “Seeing the sudden relapse of a patient in the beds next to yours can have repercussions. You may have been chatting up your fellow inmate a few seconds ago, suddenly he loses breath. You see the staff trying to revive him, failing the process and then declaring him dead. These situations can trigger panic and arouse anxiety levels.”
“Normally, a patient in ICU gets to talk to his doctors, nurses and be a part of the dialogue on his medical condition,” says Dr Punnoose. “But the Covid-19 treatment protocol prohibits any kind of humanising.”
“The ICU psychosis has always been there”, says Dr Aswin S, General Medicine (MD), BCMCH. “But in a Covid facility, when you are hooked onto a non-invasive ventilator without sedation for weeks, delirium and depression are unavoidable symptoms.”
“As a pulmonologist treating Category C patients in the government sector, my primary responsibility is to avoid deaths,” says Dr Ajai Mohan, ICU in-charge, General Hospital, Kottayam. “From the initial and mild sore throat, dry cough to the severe breathlessness and lung inflammation, priority is given to medical symptoms.”
No, doctors cannot be dismissive of withdrawal symptoms, anxiety disorders or disturbed behaviour but “hand-holding is not always practical”.
Even though mobile phones, tablets and televisions are provided, the patients do not watch light-hearted entertainment but stick to news of the pandemic. How many deaths? What are the new threats? This bias compounded by an alarmist social media adds up to the overall negativity inside a Covid ward.

No respite at home
Back home, the situation hardly improves.
Fifty-five-year-old Manoj Kumar was on an invasive ventilator with high-oxygen flow for 12 days. Since he was not conscious, his treatment went smoothly. But when he was moved to the 30-bed Isolation Ward, he started re-orientating himself slowly. Panic struck. He realised that he had lost count of days. Some beds were empty, so he knew a few patients had died. He started fighting sleep. He refused to let the nurses touch him.
His son Deepak says, “I had to take a room on the ground floor. He would call me many times on the phone. The nurses told me to get a PPE kit and they showed me to him. It was a risk. It could have made him worse and consequently affected his oxygen saturation levels again.”
Mohan Kumar is slowly regaining his physical health with daily physiotherapy sessions. “Lying prostrate for three weeks sapped the muscle strength in his legs”, says Deepak. “He cannot sleep. Even when he naps in the day-time, he doesn’t wake up with fresh energy.”
71-year-old Rajappan was admitted for five days in the Isolation Ward. He recalls that apart from chest infection and dry cough, breathlessness, his biggest trouble was lack of sleep. “I had no idea why I couldn’t sleep through the night. I was allowed to sit up, walk to the bathroom after the third day. I thought it was because I wasn’t tired enough and the sleep will return once I resume my normal working hours.”
But it has been three weeks since Rajappan re-joined duty as the supervising officer in a hollow-bricks factory. “My work entails a lot of walking, manning the loading/unloading processes on site. I am eating well. My walking speed has decreased and I find myself panting often. But I welcomed the fatigue thinking it would get me good sleep in the night. So far, it hasn’t helped.”
Sleep like a baby
Sleep patterns can be reset only through a multi-faceted approach to attaining sleep hygienic principles. “Inside a Covid ward, options are limited but beds can be positioned near the windows. Calendars and clocks can be displayed.”
At home, one must not only avoid sleeping during the day but also towards late into the morning. A uniform wake-up time should be followed daily irrespective of how late one slept. Early morning exposure to the sun is a must-have stimulant that helps the brain to reset time. Routines must go on. Prior to sleeping time, all electronic devices should be disconnected.
“Instead, boring, monotonous and conventional activities like reading, sewing, writing should precede one’s sleeping hours”.
The biggest hurdle for insomniacs is to avoid ‘catastrophic anticipation” – what if I don’t sleep tonight? – and adopt a ‘paradoxical intention’ – I do not want to sleep. I will work. It doesn’t matter.
For many, the senses of taste and smell have returned. The fatigue and lack of enthusiasm are tolerable, when at one’s own home surrounded by family. But to be the only one lying fully awake in the middle of the night – that needs to change, and fast.

