Podcast: NYT health correspondent says COVID-19 relapse unlikely

Since early April 2020, reports have been suggesting a rise in the COVID-19 relapse — recurrence of the infection in a person who had tested negative. However, experts say that relapse of COVID-19 infection is very unlikely.
In April, the WHO, in one of its daily commentaries on the issue of ‘immunity passports’, concluded, “At this point in the pandemic, there is not enough evidence about the effectiveness of antibody-mediated immunity to guarantee the accuracy of an immunity passport or risk-free certificate.”
But can a person who had been infected by COVID-19 get reinfected? “Unlikely,” says Apoorva Mandavilli, health and science reporter at The New York Times.
In her article, titled, COVID Reinfection, Can You Get COVID-19 Again? she quotes multiple researchers, including Marc Lipsitch, an epidemiologist at the T Chan School of Medicine, who concur with this view. “I haven’t heard of a case where it’s been truly unambiguously demonstrated,” Lipsitch had told the reporter.
The @voxdotcom article is a perfect example of doing what @BillHanage and I wrote in Feb. would cause trouble with COVID-19: conflating "x is possible" with "x is common." https://t.co/LXkKF6CNYX. Most would expect some reinfections: q is how often, how severe, how contagious? https://t.co/PVCorruQp7
— Marc Lipsitch (@mlipsitch) July 13, 2020
In order to understand the idea behind infections and reinfections, one needs to go back to the drawing board on immunology. What is the immune system and how does it work?
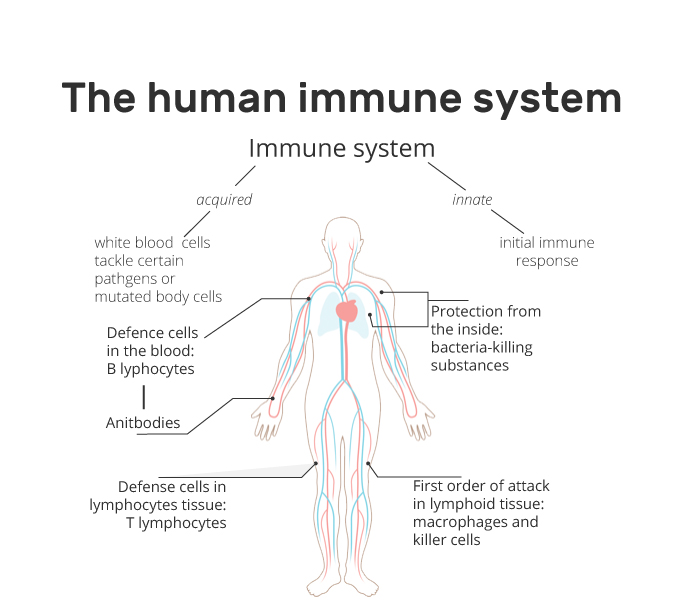
The immune system is an extremely complex network of cells and proteins that protects the human body against infection. The immune system, much like how a librarian catalogues in his library, keeps a record of every germ (microbe) it has ever defeated so it can recognise and destroy the microbe quickly if it enters the body again.
A tweetorial by Prof Akiko Iwasaki of the Yale Medical School explains the process of immunology, including the much-talked-about ‘cytokine storm’ in COVID-19.

“It (reinfection) is very unlikely. Also, it has been shown in Rhesus monkeys that they do not get reinfected,” says Prof Krishnaswami a retired professor of bioinformatics at the Madurai Kamaraj University. A 2007 study shows SARS Cov antibodies stay and SARS Cov patients are unlikely to get reinfected at least for 3 years. “Considering the relatedness and similarity between SARS-CoV and SARS-CoV-2, one would expect the same with Cov2 also,” he said.
There is an urgent need for resolving this debate at this point when many vaccine candidates are at the final stage of clinical trials. Only then the ‘belief’ that herd immunity could be achieved with a vaccine can be accepted as an article of faith.
“After the initial focus on flattening the curve, we are all now after ‘herd immunity’. Acquiring herd immunity just from natural exposure is unlikely in the short term. But, with a combination of natural infection and multiple (partially effective but safe) vaccines, we can get there,” says Dr Navaneetha Rao, a Houston-based clinical research scientist.
“Overall messaging regards CoV2 is bad and when scientists add to it, it becomes considerably worse!” he says on the topic of COVID-19 reinfection which suddenly seems to be gaining currency in various discussions and media reports.
Related Podcast: Phase 3 will determine the efficacy of the Oxford vaccine, says Dr. TS Ganesan
Also, media reports have been indicating reduced anti-body levels and anecdotal evidence at Hyderabad, India, where an antibody test conducted in July on a health care worker, who had been infected with the coronavirus, showed negative results for antibodies. This has prompted many people to ask if COVID-19 reinfection was a reality?
“The drop by itself is not alarming, if the memory cells(T) are primed to mount a quick and robust response if reinfection occurs. This underscores the need for robust, yet simple clinical studies to get to the bottom of this- example controlled challenge/re-challenge studies,” says Dr Rao.
“After the battle ends, balloon-like cells that live in the bone marrow steadily pump out a small number of specialized assassins. The next time — and every time after that — that the body comes across the virus, those cells can mass-produce antibodies within hours’, “Its normal biology” said Apoorva Mandavilli.
“Your blood carries the memory of every pathogen you’ve ever encountered. If you’ve been infected with the coronavirus, your body most likely remembers that, too” she wrote in a piece on the NYT.
Listen to The Federal‘s podcast with Apoorva Mandavilli:


