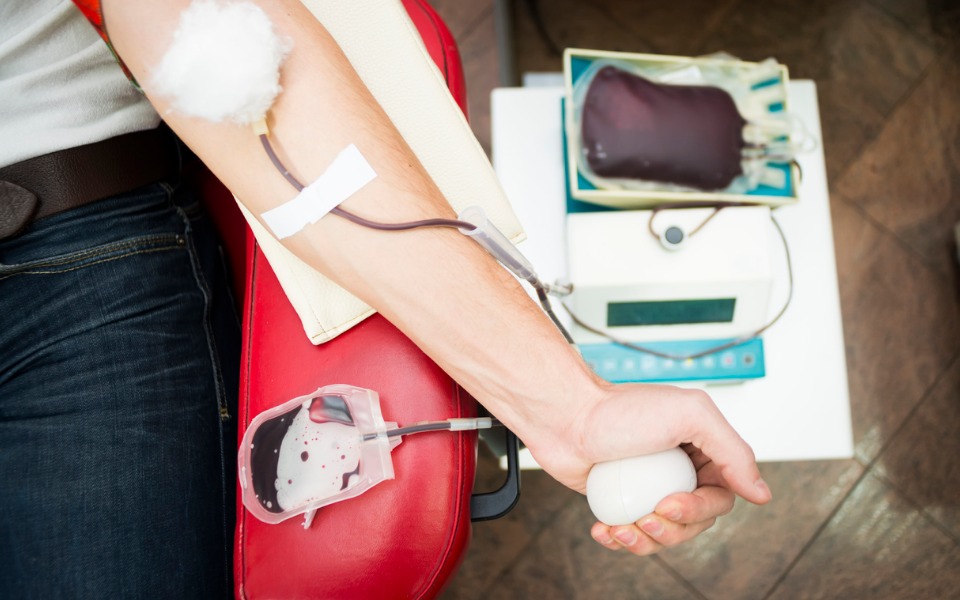
Lockdown worsens existing issues with blood donation, availability in India
How did the lockdown affect the overall health of Indians? The answer to that question depends on whom we talk about. The lockdown certainly helped avoid a large number of deaths. But what about those who were sick or those that required urgent care and attention?

How did the lockdown affect the overall health of Indians?
The answer to that question depends on whom we talk about. The lockdown certainly helped avoid a large number of deaths. But what about those who were sick or those that required urgent care and attention?
For many of them, the clock had begun to tick backward. Information now available shows that their conditions were precarious.
Hospital data reveals that the number of patients visiting them declined, both for infectious and non-communicable diseases, sometimes quite drastically. Maternal health care services were severely curtailed, child immunisation dropped across the board, lab investigations declined, treatment for tuberculosis slowed down, family planning services were disrupted, and fewer emergencies reached institutions.
Some patients need regular transfusion of blood. The lack of it turned the situation into an emergency. In effect, the lockdown disrupted the supply chain. Organisations cancelled blood donation drives. Others like the Indian Red Cross barely managed to scratch up 20 percent of the amount they usually collect on an average day. Ninety five percent of the blood in the country comes from camps organised for its collection. These numbers began to decline steeply during lockdown.
Related news: Amid COVID-19, blood shortage adds to the lockdown woes
The National Health Mission’s integrated blood bank management information system, e-RaktKosh, shows that in February 2020, the number of camps held across the country was over 470.
In April, when the lockdown was in force, that number came down to 148.
Some states did well, but others did not. Tamil Nadu, for example, had managed to organise around 20 camps during each of the first three months of the year. That number dwindled to four in April.
Gujarat did much better than Tamil Nadu, but Jammu and Kashmir’s performance was depressing. It could organise only two camps during the first few months of 2020. Overall, availability of blood became an issue during the lockdown.
Besides camps, the number of donations also influences blood availability. That number was close to 40,000 in February this year, but reduced to around 21,000 in April.
We do not have a state-wise breakdown of numbers but it would be safe to assume that there is a good amount of correspondence between the number of camps organised and the number of donations. To get a sense of what the lockdown did to the number of donations, one has to note that the number of blood donations never touched 21,000 in the year 2019.
Related news: From delivery persons to blood donors: WB cops take on various roles
Accessibility further sharpened patients’ afflictions. Those who needed blood could not get it. Blood banks became virtually inaccessible. Some of them closed shop. The authorities closed a few others. Those that were open found it difficult to operate. Either their staff or their donors were reluctant to come because of fear of infection or lack of transportation.
When it comes to blood transfusion, distance matters. It is worthwhile to remember that until last year, about 10 percent of 723 districts in the country had no blood banks.
Patients, especially children, living there had nowhere to go because of the lockdown. Donor mobilization acquired greater urgency.
On March 25, the MoHFW’s National Blood Transfusion Council issued a guidance to blood transfusion services in India in light of the COVID-19 pandemic. It observed, “If people do not turn up to donate at blood centres or camp locations, there is a likelihood of shortfall in blood supplies, which may be detrimental to those who are in urgent need of blood and blood components…” It advised them to maintain necessary precautions (such as social distancing during blood collection), ensure blood safety, and promote donor education and communication.
A fortnight later, Union health minister Dr Harsh Vardhan wrote to his counterparts in states and union territories. He said, “It may not be possible to organize blood donation camps. However, at the same time, it is necessary to ensure sufficient availability of blood, especially for people needing regular blood transfusion on account of blood disorders such as Thalassemia, Sickle Cell Anemia, Hemophilia etc.”
The lockdown brings into sharp focus the need to ramp up blood collection, distribution and utilization strategy, to motivate women to donate blood in large numbers, to increase funding of the anaemic public health system, and to dispel myths and misconceptions surrounding blood donation. As Yogesh Jain and Naman Shah of Jan Swasthya Sahyog say, “Our planning should not be judged by whether the lockdown worked or not, but by what we did with the opportunity, at what cost and for whom.”
(Pradeep Krishnatray is a former director for Research and Strategic Planning, Johns Hopkins Center for Communication Programs, New Delhi)

