
COVID-19: Scientists peer at waste for info on public health

Isn’t it surprising to know that what we flush down our toilets carries a wealth of information about our health? Raw, untreated wastewater that carries human excreta is also a reservoir of several chemicals, metabolites and pathogens that are regularly eliminated by the body.
By screening samples of the sewage, experts can estimate the concentration of compounds or the prevalence of disease-causing microbes that could be circulating in a community or region. A simple back-calculation reveals the extent of the element under surveillance. And, this is precisely how a new line of research studies are investigating further, to gain insights into how and when the novel coronavirus spread its tentacles across borders.
The primary objective of the science of public health is to prevent and treat diseases, thereby ensuring an improved quality of life of a population. In this endeavour, epidemiology plays a vital role in shaping policies and regulations. Having Greek roots, the word epidemiology translates to – ‘the study about what has come upon people’ (epi – upon, demos – people, and logos – study).
Related news: Buying a loose cigarette is risky if seller is COVID-positive
Epidemiology is an interdisciplinary field and is based on carefully designed extensive data collection of a wide range of parameters, and the rigorous statistical analysis of the collected data. The ensuing results of the analysis help determine where and how the state of public health is headed.
Epidemiological models are all the more critical during disease outbreaks, such as the present pandemic situation. They are invaluable tools that help in investigating and monitoring disease transmission and progression, clinical trials, research, and disease investigation. Such insights help frame regulations and safety measures for public health and wellbeing. Several models were proposed in the past few months that influenced the disease propagation across borders
Wastewater-based epidemiology
Our body regularly eliminates many chemicals, metabolites and pathogens through urine and excreta. Screening the waste matter is a proven clinical method (stool and urine tests) to assess diseases, health status or the presence of drugs and toxic chemicals. Apart from medical reasons, we see such assessment methods commonly in the field of sports for drug testing.
By using similar leverage, new science is emerging called Wastewater-Based Epidemiology (WBE). By collecting and screening untreated wastewater samples periodically, WBE looks for clues called biomarkers that give inputs about the health status of a population in a region.
By employing this clever tactic of mass analyses, experts get a community-level picture of the prevalence of the element under surveillance.
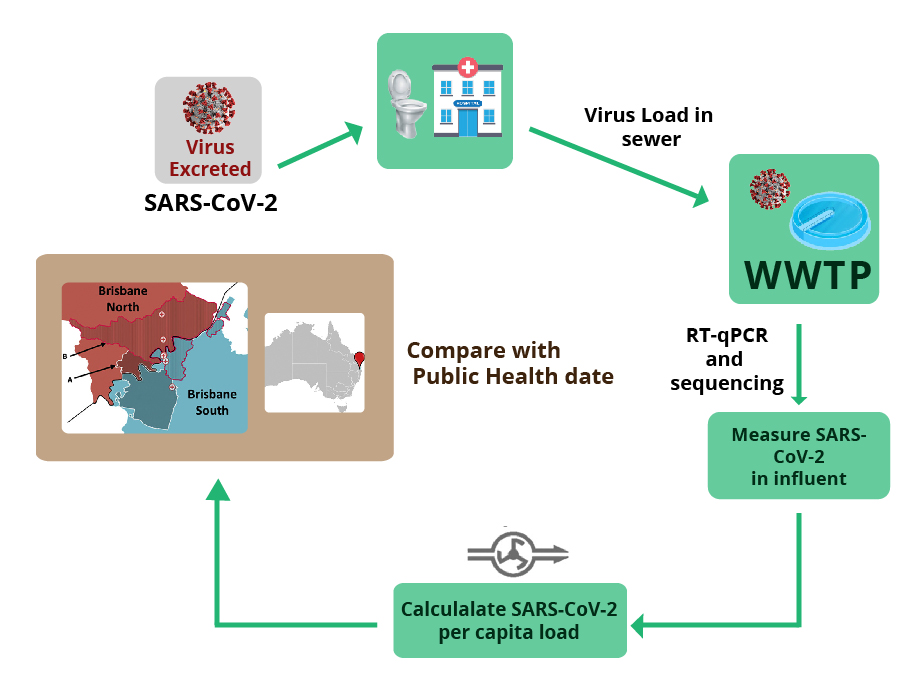
WBE relies on multidisciplinary expertise: specially designed sensors, chemical analysis techniques and biological assays. Experts can quickly detect chemicals and their metabolites (such as illicit drugs), or presence of pathogens such as bacteria and viruses that get flushed into the drains. After determining the levels of the elements under scrutiny, a reverse analysis and extrapolation over the population density reveal the levels of contamination.
The results are integrated over time and across regions. This helps to keep an eye on the circulation of the contaminant and its levels, from which they can derive meaningful results that can impact policymaking.
“WBE is a powerful tool to detect the extent of the presence of viruses in the community and to identify hotspots,” opines Dr. Gautam Menon, Professor, Departments of Physics and Biology, Ashoka University, Sonepat. It provides a means to identify the prevalence of the disease that might not have registered in more traditional ways of finding cases that rely on self-reporting, he adds.
What Italy has to say
Italy detected its first case of COVID-19 by the end of January. However, a recent study by Italian scientists had revealed a different story: the virus had infiltrated into the country weeks before the first case was detected. Wastewater screening enabled them to come to this conclusion.
The Italian National Institute of Health collected 40 sewage samples between October 2019 and February 2020. They performed assays on the samples to detect the novel coronavirus SARS COV-2. The team was surprised to find the presence of the virus as far back as December 2019 – two weeks even before the first reported COVID-19 case from Wuhan, China. This was a clear indication that the virus was circulating among people well before it was actually detected through symptomatic patients.
The study prompted the Italian government to launch a real-time pilot study to monitor and scrutinize the wastewaters specifically around tourist areas.
Related news: No fairytales to tell: COVID-19 spins nightmares for expecting mothers
“It would be a very useful exercise to examine old wastewater samples – if they were collected at all – in India as well, to see whether the same situation exists here too,” says Prof. Menon. Such sampling could provide valuable epidemiological inputs. “Some significant parameters could be the possibility of a larger fraction of positive cases from serological studies; or, it may give insights into immunity levels in the population,” he says.
WBE was proposed in the early 2000s and gained ground as a reliable method by 2005. Several western nations are increasingly adopting these techniques to ensure public health and safety.
Wastewater analysis can be a powerful tool to predict the onset of infectious diseases. Probability of outbreaks can be detected earlier on, compared to conventional clinical testing, which usually happens after the disease manifests in the community. Research studies indicate that miniature, ultra-sensitive sensors can be incorporated along the line of flow of the wastewater to achieve a real-time, rapid response tool.
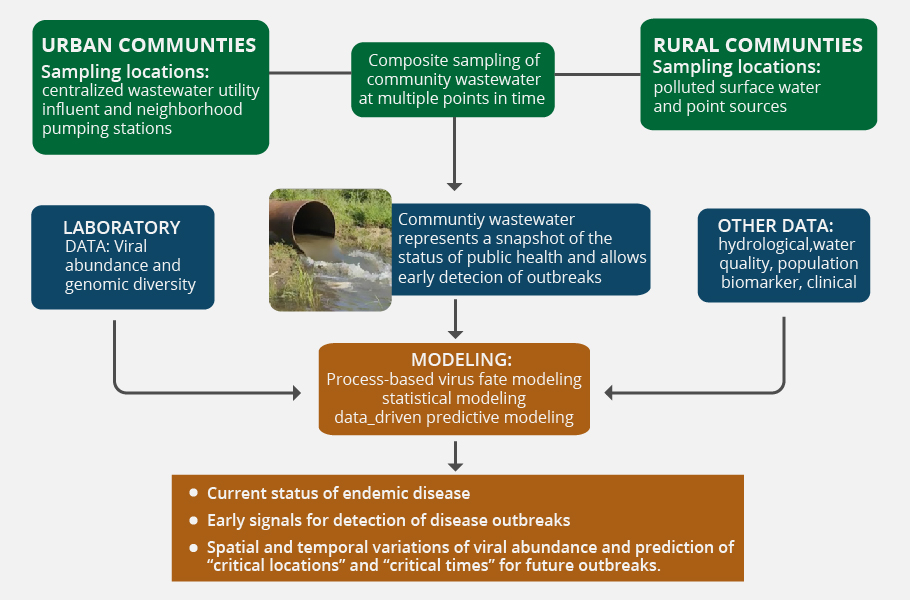
Inline biosensors are tiny specialized devices designed to test the presence of specific types of DNA, RNA, antibody or an antigen in wastewater at the treatment site. These devices generate a signal and alert the monitoring agencies when any of the designed markers are detected in the treatment of water tanks.
Can the virus spread through water?
Viruses occupy the lowest rung of the ecosystem, existing as entities or particles – neither living nor non-living. They depend on a living host cell to proliferate. In the case of the present coronavirus, a technical brief from the World Health Organization (WHO) clarifies that there is no concrete evidence of the virus surviving in drinking water or sewage. “The detected viral presence in sewage waters is only the remnants of the RNA of the virus, which definitely does not contribute to infection or the disease spread,” asserts Vishwanath S, Adjunct Professor, Azim Premji University, Bengaluru, and Trustee, Biome Environmental Trust, Bengaluru.
Also, as the COVID-19 virus is an enveloped virus, its outer, thin lipid layer is fragile and highly sensitive to disinfectants such as chlorine. As the outer protective layer degenerates, the virus becomes denatured, rendering the virus inactive. Conventional water treatment methods would suffice to deactivate the virus.
Related news: Hope and positivity to guide the way in fight against COVID-19
“In addition, the guidelines issued by WHO, CDC and India’s Central Public Health and Environmental Engineering Organization (CPHEEO) have sent an advisory to increase residual chlorine in drinking water to 0.5 mg/l, that is 2.5 times normal dosage and also to chlorinate treated wastewater for disinfection,” adds Professor Vishwanath.
Moreover, studies indicate that temperature plays a crucial role in the survival of the virus in water. Hence practices such as boiling or UV filtration methods would keep the drinking water safe. As the virus transmits predominantly through droplets, preventive measures would help arrest its spread.


